Healthcare has more digital tools than ever – yet data fragmentation remains one of the biggest barriers to performance. The root cause is familiar: multiple, siloed systems across wards, departments, and care settings that don’t share information reliably.
When data is fragmented, the impacts are predictable: clinicians waste time chasing context, patients repeat their story, reporting becomes slow and disputed, and AI initiatives stall because the foundations aren’t ready.
Digital health maturity is not the number of systems you own. It’s the ability to run high-performing workflows, produce trusted data, and build organisational trust – clinically, operationally, and technologically.
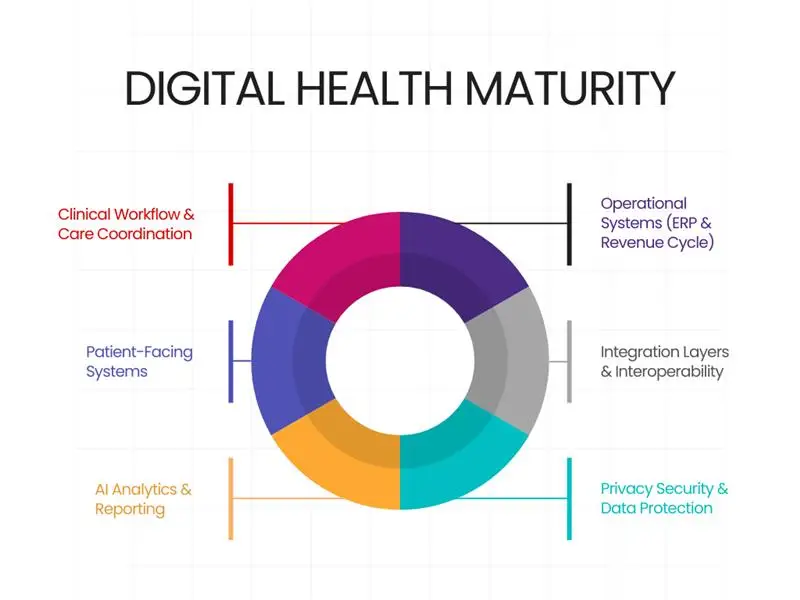
A practical way to assess this is across six maturity areas.
A 6-Category Digital Health Maturity Assessment
1) Clinical Workflow & Care Coordination
Outcome: safer care, lower clinician burden, better coordination.
Why it matters: Fragmented information breaks coordination. Mature organisations reduce handoffs, duplication, and “chart chasing” by enabling a longitudinal care record – a continuous, patient-centred view across touchpoints (ED, inpatient, outpatient, community and allied care). That longitudinal view is what turns “digital documentation” into coordinated care.
What to look for
- Clinical workflows designed to reduce rework and manual charting.
- Data captured once and reused across the journey (orders, meds, results, discharge).
- Care teams can quickly access a longitudinal view, not just an episode snapshot.
- AI used pragmatically to reduce admin load inside the workflow (summaries, drafting, prioritisation), with oversight.
Systems in scope: EMR/EHR, RIS, pharmacy, LIS, other clinical systems.
2) Operational Systems (ERP & Revenue Cycle)
Outcome: financial sustainability, improved throughput, less leakage and rework.
Why it matters: Operational maturity is where digital investment becomes measurable. When core operational systems are automated and consistent, you see fewer billing errors, faster patient flow, and reduced costs.
What to look for
- Accurate real-time ADT/bed visibility and patient flow.
- Revenue cycle automation and validation (prevent issues rather than correcting later).
- Scheduling aligned to demand, workforce, and physical assets.
- Supply chain visibility that reduces stock-outs, waste, and substitution risk.
Systems in scope: ADT/BMS, finance & billing, scheduling, supply chain, facilities/HR.
3) Patient-Facing Systems
Outcome: better access, improved experience, lower admin load.
Why it matters: Patients experience fragmentation directly – repeating details, filling forms multiple times, unclear status updates. Mature “digital front doors” reduce friction by making the journey simpler and more connected.
What to look for
- Self-service access: bookings, forms, consent, payments, updates.
- Two-way communication that reduces inbound calls and missed appointments.
- Remote monitoring integrated into defined care pathways (with escalation ownership).
- Patient experience connected to the broader record – not isolated in a portal silo.
Systems in scope: mobile apps, patient portals, remote patient monitoring.
4) Integration Layers & Interoperability
Outcome: less duplication, fewer errors, faster ecosystem coordination.
Why it matters: Data fragmentation is fundamentally an integration problem. Multiple systems across care settings create silos unless interoperability is designed deliberately. Mature organisations treat integration as core infrastructure using standards and governance, not a series of one-off interfaces.
What to look for
- Reliable internal data flow between departments and systems.
- Standards-based interoperability using FHIR and APIs.
- Monitoring and ownership for integration health (failures detected early).
- External exchange that supports continuity of care across partners and settings.
- Integration that enables longitudinal records—so care teams can work with complete context.
Components in scope: interface engines/APIs, HIE.
5) AI, Analytics & Reporting
Outcome: faster decisions, earlier intervention, measurable performance improvement.
Why it matters: AI won’t fix fragmented data. To unlock real value, organisations need foundational data quality and integration first. Advanced analytics and AI depend on trusted inputs and they deliver results only when embedded into workflows and supported by process design.
What to look for
- A governed data foundation (common definitions, lineage, ownership).
- High-quality, integrated data that is fit for analytics and AI.
- Operational dashboards that enable action now, not retrospective debate.
- Predictive analytics that is validated, monitored, and clinically safe.
- AI adoption focused on process-oriented thinking and workflow automation first, then advanced models layered on top.
Key principle: The fastest path to AI value is usually workflow automation + strong data foundations, not standalone pilots.
Capabilities in scope: AI-integrated workflows, predictive analytics, operational/statutory reporting.
6) Privacy, Security & Data Protection
Outcome: trust, compliance, resilience—and the ability to innovate safely.
Why it matters: Innovation without trust doesn’t scale. Privacy, consent, and security must be embedded into the platform—especially as data sharing increases and AI expands access to sensitive information.
What to look for
- Consent management implemented consistently across the patient journey.
- Privacy-by-design controls that align to governance and regulatory obligations.
- A zero trust approach that assumes breach and limits blast radius.
- Strong IAM (least privilege, MFA, access reviews).
- Proven resilience: high availability and disaster recovery tested with measurable targets.
Capabilities in scope: consent management, zero trust, IAM, HA/DR.
If you want maturity and AI value, you don’t start with more tools. You start with:
- reducing fragmentation through integration and interoperability
- establishing longitudinal records for coordinated care
- improving foundational data quality and governance
- designing workflows and automation that reduce burden
- embedding privacy, consent, and zero trust so innovation can scale safely
Digital health maturity is an operating model upgrade. It shows up in better clinical flow, trusted reporting, lower risk, and a patient journey that feels connected, not fragmented.
Take the 10-Minute Organisational Digital Health Maturity Assessment to benchmark your clinical, operational, and data capabilities against standards. Get a tailored roadmap to move from Functional to Leading.



